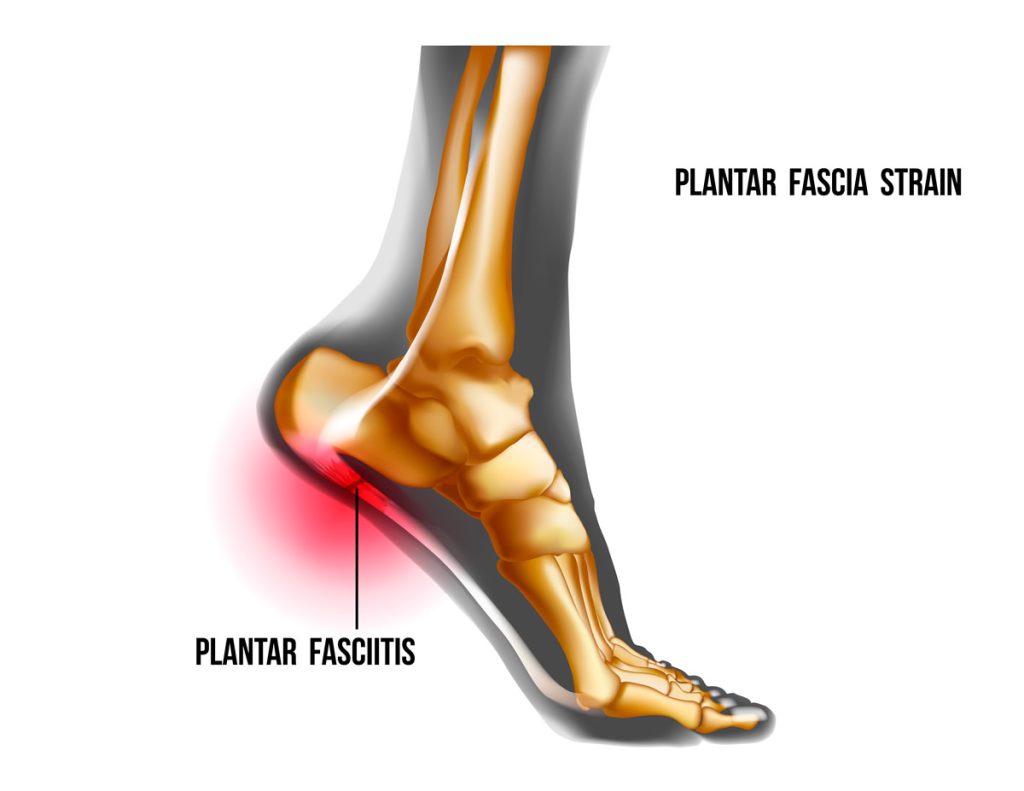
Busy routines become harder to maintain when heel pain follows nearly every step. Activities that once felt normal, including walking, exercising, standing at work, or climbing stairs, can slowly become frustrating with ongoing plantar fasciitis symptoms. Proper treatment from a podiatrist in Decatur AL often focuses on reducing stress across the foot before secondary problems begin affecting the rest of the body.
Altered Walking Patterns
Protective limping usually develops naturally when people try avoiding pressure on painful heels. Small changes in walking form may not seem serious at first, but uneven movement can shift body weight into unhealthy positions throughout the day. Continuous imbalance often forces muscles and joints to compensate in ways they were never designed to handle.
Extended gait changes sometimes create fatigue even during simple activities like grocery shopping or standing in line. Several patients visiting a Decatur podiatrist notice soreness developing on the opposite foot because extra weight transfers unevenly while walking. Persistent strain may eventually affect balance, posture, and overall comfort during daily movement.
Pain Beyond the Foot
Heel pain rarely stays isolated when plantar fasciitis remains untreated for long periods. Tight muscles and altered posture can spread discomfort upward into the ankles, knees, hips, and lower back. Ongoing compensation frequently places extra stress on joints already handling repeated movement throughout the day.
Athletes and active workers commonly experience secondary soreness because the body constantly adjusts to avoid heel pressure. Chronic discomfort sometimes reduces mobility even when the original foot pain seems manageable. Experienced plantar fasciitis specialist evaluations often examine surrounding joints to identify related movement problems connected to the condition.
Thickened Fascia Tissue
Repeated inflammation may cause the plantar fascia ligament to thicken over time as the body reacts to constant strain. Scar tissue can gradually reduce flexibility beneath the foot, making walking feel tighter and less natural. Reduced elasticity sometimes increases discomfort during exercise, stair climbing, or long work shifts.
Long-term tissue changes may also slow recovery because stiff fascia absorbs force less effectively during movement. Several people seeking a plantar fasciitis doctor discover that untreated irritation lasting months or years creates deeper structural problems beneath the arch. Consistent treatment often helps limit excessive thickening before mobility declines further.
Heel Spurs and Bone Stress
Bony growths known as heel spurs occasionally develop where the fascia repeatedly pulls against the heel bone. Extra pressure along the attachment point may trigger small calcium deposits over time. Many individuals with plantar fasciitis experience heel spurs alongside chronic inflammation beneath the foot. Sharp pain does not always come directly from the spur itself, but surrounding irritation frequently worsens discomfort during standing and walking. Active lifestyles may become difficult when both inflammation and bone stress remain untreated together. Reliable care from a podiatrist in Decatur AL can help determine whether heel spurs contribute to worsening symptoms.
Risk of Fascia Tears
Overloaded fascia tissue sometimes weakens enough to partially tear during sports, running, or sudden movement. Small tears may create swelling, bruising, or sharp pain that feels different from normal plantar fasciitis soreness. Severe strain often develops after people continue high-impact activity despite ongoing heel discomfort.
Athletic training without proper recovery may increase the likelihood of tissue damage beneath the arch. Several plantar fasciitis specialist treatment plans focus on lowering tension before tearing occurs. Supportive footwear, stretching, and activity adjustments frequently help reduce excessive stress across vulnerable tissue.
Declining Physical Endurance
Reduced movement often becomes one of the hidden effects of chronic heel pain. Exercise routines may slowly disappear because walking, jogging, or standing feels exhausting after prolonged discomfort. Lower activity levels can gradually affect stamina, cardiovascular health, and overall physical conditioning.
Daily frustration sometimes leads people to avoid recreational hobbies they once enjoyed regularly. Extended inactivity may also contribute to weight gain, which places even more pressure on painful heels. Trusted Decatur podiatrist evaluations commonly address fitness limitations connected to long-term plantar fasciitis symptoms.
Tight Ankles and Calves
Restricted ankle flexibility frequently develops alongside chronic plantar fasciitis because lower leg muscles tighten in response to altered walking patterns. Limited mobility may increase pulling force across the heel every time the foot contacts the ground. Reduced flexibility often makes morning movement especially uncomfortable.
Stiff calf muscles can also affect balance and walking efficiency during physically demanding work or exercise. Consistent stretching programs sometimes improve mobility while lowering repeated strain beneath the arch. Many patients working with a plantar fasciitis doctor notice better comfort after improving lower leg flexibility.
Sleep Disruption and Instability
Nighttime throbbing occasionally interrupts sleep when inflammation remains active after long days of standing or walking. Poor rest may reduce recovery while increasing fatigue during daytime activity. Ongoing discomfort sometimes creates frustration that affects concentration, mood, and daily productivity.
Uneven walking combined with soreness can also increase the risk of slipping or losing balance on stairs, wet flooring, or uneven surfaces. Active individuals dealing with plantar fasciitis often underestimate how quickly instability develops from constant limping. The Foot Clinic helps patients understand how heel pain influences far more than the foot itself by addressing movement problems, flexibility loss, and long-term strain connected to plantar fasciitis before everyday activity becomes harder to manage.